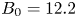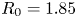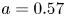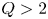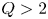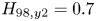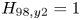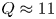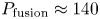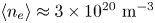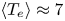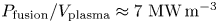45 results
The mediating role of health behaviors in the association between depression, anxiety and cancer incidence: an individual participant data meta-analysis
- Kuan-Yu Pan, Lonneke van Tuijl, Maartje Basten, Judith J. M. Rijnhart, Alexander de Graeff, Joost Dekker, Mirjam I. Geerlings, Adriaan Hoogendoorn, Adelita V. Ranchor, Roel Vermeulen, Lützen Portengen, Adri C. Voogd, Jessica Abell, Philip Awadalla, Aartjan T. F. Beekman, Ottar Bjerkeset, Andy Boyd, Yunsong Cui, Philipp Frank, Henrike Galenkamp, Bert Garssen, Sean Hellingman, Monika Hollander, Martijn Huisman, Anke Huss, Melanie R. Keats, Almar A. L. Kok, Steinar Krokstad, Flora E. van Leeuwen, Annemarie I. Luik, Nolwenn Noisel, Yves Payette, Brenda W. J. H. Penninx, Susan Picavet, Ina Rissanen, Annelieke M. Roest, Judith G. M. Rosmalen, Rikje Ruiter, Robert A. Schoevers, David Soave, Mandy Spaan, Andrew Steptoe, Karien Stronks, Erik R. Sund, Ellen Sweeney, Alison Teyhan, Emma L. Twait, Kimberly D. van der Willik, Femke Lamers
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 29 April 2024, pp. 1-14
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Although behavioral mechanisms in the association among depression, anxiety, and cancer are plausible, few studies have empirically studied mediation by health behaviors. We aimed to examine the mediating role of several health behaviors in the associations among depression, anxiety, and the incidence of various cancer types (overall, breast, prostate, lung, colorectal, smoking-related, and alcohol-related cancers).
MethodsTwo-stage individual participant data meta-analyses were performed based on 18 cohorts within the Psychosocial Factors and Cancer Incidence consortium that had a measure of depression or anxiety (N = 319 613, cancer incidence = 25 803). Health behaviors included smoking, physical inactivity, alcohol use, body mass index (BMI), sedentary behavior, and sleep duration and quality. In stage one, path-specific regression estimates were obtained in each cohort. In stage two, cohort-specific estimates were pooled using random-effects multivariate meta-analysis, and natural indirect effects (i.e. mediating effects) were calculated as hazard ratios (HRs).
ResultsSmoking (HRs range 1.04–1.10) and physical inactivity (HRs range 1.01–1.02) significantly mediated the associations among depression, anxiety, and lung cancer. Smoking was also a mediator for smoking-related cancers (HRs range 1.03–1.06). There was mediation by health behaviors, especially smoking, physical inactivity, alcohol use, and a higher BMI, in the associations among depression, anxiety, and overall cancer or other types of cancer, but effects were small (HRs generally below 1.01).
ConclusionsSmoking constitutes a mediating pathway linking depression and anxiety to lung cancer and smoking-related cancers. Our findings underline the importance of smoking cessation interventions for persons with depression or anxiety.
Can we check serum lithium levels less often without compromising patient safety?
- Adrian H. Heald, David Holland, Michael Stedman, Mark Davies, Chris J. Duff, Ceri Parfitt, Lewis Green, Jonathan Scargill, David Taylor, Anthony A. Fryer
-
- Journal:
- BJPsych Open / Volume 8 / Issue 1 / January 2022
- Published online by Cambridge University Press:
- 17 December 2021, e18
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Lithium is viewed as the first-line long-term treatment for prevention of relapse in people with bipolar disorder.
AimsThis study examined factors associated with the likelihood of maintaining serum lithium levels within the recommended range and explored whether the monitoring interval could be extended in some cases.
MethodWe included 46 555 lithium rest requests in 3371 individuals over 7 years from three UK centres. Using lithium results in four categories (<0.4 mmol/L; 0.40–0.79 mmol/L; 0.80–0.99 mmol/L; ≥1.0 mmol/L), we determined the proportion of instances where lithium results remained stable or switched category on subsequent testing, considering the effects of age, duration of lithium therapy and testing history.
ResultsFor tests within the recommended range (0.40–0.99 mmol/L categories), 84.5% of subsequent tests remained within this range. Overall, 3 monthly testing was associated with 90% of lithium results remaining within range, compared with 85% at 6 monthly intervals. In cases where the lithium level in the previous 12 months was on target (0.40–0.79 mmol/L; British National Formulary/National Institute for Health and Care Excellence criteria), 90% remained within the target range at 6 months. Neither age nor duration of lithium therapy had any significant effect on lithium level stability. Levels within the 0.80–0.99 mmol/L category were linked to a higher probability of moving to the ≥1.0 mmol/L category (10%) compared with those in the 0.4–0.79 mmol/L group (2%), irrespective of testing frequency.
ConclusionWe propose that for those who achieve 12 months of lithium tests within the 0.40–0.79 mmol/L range, the interval between tests could increase to 6 months, irrespective of age. Where lithium levels are 0.80–0.99 mmol/L, the test interval should remain at 3 months. This could reduce lithium test numbers by 15% and costs by ~$0.4 m p.a.
Maternal diet high in linoleic acid alters offspring fatty acids and cardiovascular function in a rat model
- Nirajan Shrestha, Simone Sleep, Tessa Helman, Olivia Holland, James S. M. Cuffe, Anthony V. Perkins, Andrew J. McAinch, John P. Headrick, Deanne H. Hryciw
-
- Journal:
- British Journal of Nutrition / Volume 127 / Issue 4 / 28 February 2022
- Published online by Cambridge University Press:
- 16 April 2021, pp. 540-553
- Print publication:
- 28 February 2022
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Linoleic acid (LA), an essential n-6 fatty acid (FA), is critical for fetal development. We investigated the effects of maternal high LA (HLA) diet on offspring cardiac development and its relationship to circulating FA and cardiovascular function in adolescent offspring, and the ability of the postnatal diet to reverse any adverse effects. Female Wistar Kyoto rats were fed low LA (LLA; 1·44 % energy from LA) or high LA (HLA; 6·21 % energy from LA) diets for 10 weeks before pregnancy and during gestation/lactation. Offspring, weaned at postnatal day 25, were fed LLA or HLA diets and euthanised at postnatal day 40 (n 6–8). Maternal HLA diet decreased circulating total cholesterol and HDL-cholesterol in females and decreased total plasma n-3 FA in males, while maternal and postnatal HLA diets decreased total plasma n-3 FA in females. α-Linolenic acid (ALA) and EPA were decreased by postnatal but not maternal HLA diets in both sexes. Maternal and postnatal HLA diets increased total plasma n-6 and LA, and a maternal HLA diet increased circulating leptin, in both male and female offspring. Maternal HLA decreased slopes of systolic and diastolic pressure–volume relationship (PVR), and increased cardiac Col1a1, Col3a1, Atp2a1 and Notch1 in males. Maternal and postnatal HLA diets left-shifted the diastolic PVR in female offspring. Coronary reactivity was altered in females, with differential effects on flow repayment after occlusion. Thus, maternal HLA diets impact lipids, FA and cardiac function in offspring, with postnatal diet modifying FA and cardiac function in the female offspring.
Establishing diagnostic thresholds for Alzheimer's disease in adults with Down syndrome: the Cambridge Examination for Mental Disorders of Older People with Down's Syndrome and Others with Intellectual Disabilities (CAMDEX-DS)
- Jessica A. Beresford-Webb, Elijah Mak, Monika Grigorova, Samuel J. Daffern, Anthony J. Holland, Shahid H. Zaman
-
- Journal:
- BJPsych Open / Volume 7 / Issue 3 / May 2021
- Published online by Cambridge University Press:
- 13 April 2021, e79
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Diagnosis of prodromal Alzheimer's disease and Alzheimer's disease dementia in people with Down syndrome is a major challenge. The Cambridge Examination for Mental Disorders of Older People with Down's Syndrome and Others with Intellectual Disabilities (CAMDEX-DS) has been validated for diagnosing prodromal Alzheimer's disease and Alzheimer's disease dementia, but the diagnostic process lacks guidance.
AimsTo derive CAMDEX-DS informant interview threshold scores to enable accurate diagnosis of prodromal Alzheimer's disease and Alzheimer's disease dementia in adults with Down syndrome.
MethodPsychiatrists classified participants with Down syndrome into no dementia, prodromal Alzheimer's disease and Alzheimer's disease dementia groups. Receiver operating characteristic analyses assessed the diagnostic accuracy of CAMDEX-DS informant interview-derived scores. Spearman partial correlations investigated associations between CAMDEX-DS scores, regional Aβ binding (positron emission tomography) and regional cortical thickness (magnetic resonance imaging).
ResultsDiagnostic performance of CAMDEX-DS total scores were high for Alzheimer's disease dementia (area under the curve (AUC), 0.998; 95% CI 0.953–0.999) and prodromal Alzheimer's disease (AUC = 0.954; 95% CI 0.887–0.982) when compared with healthy adults with Down syndrome. When compared with those with mental health conditions but no Alzheimer's disease, CAMDEX-DS Section B scores, denoting memory and orientation ability, accurately diagnosed Alzheimer's disease dementia (AUC = 0.958; 95% CI 0.892–0.984), but were unable to diagnose prodromal Alzheimer's disease. CAMDEX-DS total scores exhibited moderate correlations with cortical Aβ (r ~ 0.4 to 0.6, P ≤ 0.05) and thickness (r ~ −0.4 to −0.44, P ≤ 0.05) in specific regions.
ConclusionsCAMDEX-DS total score accurately diagnoses Alzheimer's disease dementia and prodromal Alzheimer's disease in healthy adults with Down syndrome.
Neutron Star Extreme Matter Observatory: A kilohertz-band gravitational-wave detector in the global network
- Part of
- K. Ackley, V. B. Adya, P. Agrawal, P. Altin, G. Ashton, M. Bailes, E. Baltinas, A. Barbuio, D. Beniwal, C. Blair, D. Blair, G. N. Bolingbroke, V. Bossilkov, S. Shachar Boublil, D. D. Brown, B. J. Burridge, J. Calderon Bustillo, J. Cameron, H. Tuong Cao, J. B. Carlin, S. Chang, P. Charlton, C. Chatterjee, D. Chattopadhyay, X. Chen, J. Chi, J. Chow, Q. Chu, A. Ciobanu, T. Clarke, P. Clearwater, J. Cooke, D. Coward, H. Crisp, R. J. Dattatri, A. T. Deller, D. A. Dobie, L. Dunn, P. J. Easter, J. Eichholz, R. Evans, C. Flynn, G. Foran, P. Forsyth, Y. Gai, S. Galaudage, D. K. Galloway, B. Gendre, B. Goncharov, S. Goode, D. Gozzard, B. Grace, A. W. Graham, A. Heger, F. Hernandez Vivanco, R. Hirai, N. A. Holland, Z. J. Holmes, E. Howard, E. Howell, G. Howitt, M. T. Hübner, J. Hurley, C. Ingram, V. Jaberian Hamedan, K. Jenner, L. Ju, D. P. Kapasi, T. Kaur, N. Kijbunchoo, M. Kovalam, R. Kumar Choudhary, P. D. Lasky, M. Y. M. Lau, J. Leung, J. Liu, K. Loh, A. Mailvagan, I. Mandel, J. J. McCann, D. E. McClelland, K. McKenzie, D. McManus, T. McRae, A. Melatos, P. Meyers, H. Middleton, M. T. Miles, M. Millhouse, Y. Lun Mong, B. Mueller, J. Munch, J. Musiov, S. Muusse, R. S. Nathan, Y. Naveh, C. Neijssel, B. Neil, S. W. S. Ng, V. Oloworaran, D. J. Ottaway, M. Page, J. Pan, M. Pathak, E. Payne, J. Powell, J. Pritchard, E. Puckridge, A. Raidani, V. Rallabhandi, D. Reardon, J. A. Riley, L. Roberts, I. M. Romero-Shaw, T. J. Roocke, G. Rowell, N. Sahu, N. Sarin, L. Sarre, H. Sattari, M. Schiworski, S. M. Scott, R. Sengar, D. Shaddock, R. Shannon, J. SHI, P. Sibley, B. J. J. Slagmolen, T. Slaven-Blair, R. J. E. Smith, J. Spollard, L. Steed, L. Strang, H. Sun, A. Sunderland, S. Suvorova, C. Talbot, E. Thrane, D. Töyrä, P. Trahanas, A. Vajpeyi, J. V. van Heijningen, A. F. Vargas, P. J. Veitch, A. Vigna-Gomez, A. Wade, K. Walker, Z. Wang, R. L. Ward, K. Ward, S. Webb, L. Wen, K. Wette, R. Wilcox, J. Winterflood, C. Wolf, B. Wu, M. Jet Yap, Z. You, H. Yu, J. Zhang, J. Zhang, C. Zhao, X. Zhu
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 37 / 2020
- Published online by Cambridge University Press:
- 05 November 2020, e047
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Gravitational waves from coalescing neutron stars encode information about nuclear matter at extreme densities, inaccessible by laboratory experiments. The late inspiral is influenced by the presence of tides, which depend on the neutron star equation of state. Neutron star mergers are expected to often produce rapidly rotating remnant neutron stars that emit gravitational waves. These will provide clues to the extremely hot post-merger environment. This signature of nuclear matter in gravitational waves contains most information in the 2–4 kHz frequency band, which is outside of the most sensitive band of current detectors. We present the design concept and science case for a Neutron Star Extreme Matter Observatory (NEMO): a gravitational-wave interferometer optimised to study nuclear physics with merging neutron stars. The concept uses high-circulating laser power, quantum squeezing, and a detector topology specifically designed to achieve the high-frequency sensitivity necessary to probe nuclear matter using gravitational waves. Above 1 kHz, the proposed strain sensitivity is comparable to full third-generation detectors at a fraction of the cost. Such sensitivity changes expected event rates for detection of post-merger remnants from approximately one per few decades with two A+ detectors to a few per year and potentially allow for the first gravitational-wave observations of supernovae, isolated neutron stars, and other exotica.
Overview of the SPARC tokamak
- Part of
- A. J. Creely, M. J. Greenwald, S. B. Ballinger, D. Brunner, J. Canik, J. Doody, T. Fülöp, D. T. Garnier, R. Granetz, T. K. Gray, C. Holland, N. T. Howard, J. W. Hughes, J. H. Irby, V. A. Izzo, G. J. Kramer, A. Q. Kuang, B. LaBombard, Y. Lin, B. Lipschultz, N. C. Logan, J. D. Lore, E. S. Marmar, K. Montes, R. T. Mumgaard, C. Paz-Soldan, C. Rea, M. L. Reinke, P. Rodriguez-Fernandez, K. Särkimäki, F. Sciortino, S. D. Scott, A. Snicker, P. B. Snyder, B. N. Sorbom, R. Sweeney, R. A. Tinguely, E. A. Tolman, M. Umansky, O. Vallhagen, J. Varje, D. G. Whyte, J. C. Wright, S. J. Wukitch, J. Zhu, the SPARC Team
-
- Journal:
- Journal of Plasma Physics / Volume 86 / Issue 5 / October 2020
- Published online by Cambridge University Press:
- 29 September 2020, 865860502
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
The SPARC tokamak is a critical next step towards commercial fusion energy. SPARC is designed as a high-field (
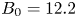 $B_0 = 12.2$ T), compact (
$B_0 = 12.2$ T), compact (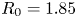 $R_0 = 1.85$ m,
$R_0 = 1.85$ m, 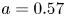 $a = 0.57$ m), superconducting, D-T tokamak with the goal of producing fusion gain
$a = 0.57$ m), superconducting, D-T tokamak with the goal of producing fusion gain 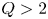 $Q>2$ from a magnetically confined fusion plasma for the first time. Currently under design, SPARC will continue the high-field path of the Alcator series of tokamaks, utilizing new magnets based on rare earth barium copper oxide high-temperature superconductors to achieve high performance in a compact device. The goal of
$Q>2$ from a magnetically confined fusion plasma for the first time. Currently under design, SPARC will continue the high-field path of the Alcator series of tokamaks, utilizing new magnets based on rare earth barium copper oxide high-temperature superconductors to achieve high performance in a compact device. The goal of 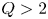 $Q>2$ is achievable with conservative physics assumptions (
$Q>2$ is achievable with conservative physics assumptions (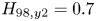 $H_{98,y2} = 0.7$) and, with the nominal assumption of
$H_{98,y2} = 0.7$) and, with the nominal assumption of 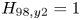 $H_{98,y2} = 1$, SPARC is projected to attain
$H_{98,y2} = 1$, SPARC is projected to attain 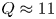 $Q \approx 11$ and
$Q \approx 11$ and 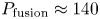 $P_{\textrm {fusion}} \approx 140$ MW. SPARC will therefore constitute a unique platform for burning plasma physics research with high density (
$P_{\textrm {fusion}} \approx 140$ MW. SPARC will therefore constitute a unique platform for burning plasma physics research with high density (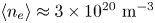 $\langle n_{e} \rangle \approx 3 \times 10^{20}\ \textrm {m}^{-3}$), high temperature (
$\langle n_{e} \rangle \approx 3 \times 10^{20}\ \textrm {m}^{-3}$), high temperature (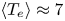 $\langle T_e \rangle \approx 7$ keV) and high power density (
$\langle T_e \rangle \approx 7$ keV) and high power density (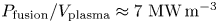 $P_{\textrm {fusion}}/V_{\textrm {plasma}} \approx 7\ \textrm {MW}\,\textrm {m}^{-3}$) relevant to fusion power plants. SPARC's place in the path to commercial fusion energy, its parameters and the current status of SPARC design work are presented. This work also describes the basis for global performance projections and summarizes some of the physics analysis that is presented in greater detail in the companion articles of this collection.
$P_{\textrm {fusion}}/V_{\textrm {plasma}} \approx 7\ \textrm {MW}\,\textrm {m}^{-3}$) relevant to fusion power plants. SPARC's place in the path to commercial fusion energy, its parameters and the current status of SPARC design work are presented. This work also describes the basis for global performance projections and summarizes some of the physics analysis that is presented in greater detail in the companion articles of this collection.
Obsessive-compulsive disorder in the elderly: A report from the International College of Obsessive-Compulsive Spectrum Disorders (ICOCS)
- B. Dell’Osso, B. Benatti, C.I. Rodriguez, C. Arici, C. Palazzo, A.C. Altamura, E. Hollander, N. Fineberg, D.J. Stein, H. Nicolini, N. Lanzagorta, D. Marazziti, S. Pallanti, M. Van Ameringen, C. Lochner, O. Karamustafalioglu, L. Hranov, M. Figee, L. Drummond, J. Grant, D. Denys, D. Cath, J.M. Menchon, J. Zohar
-
- Journal:
- European Psychiatry / Volume 45 / September 2017
- Published online by Cambridge University Press:
- 23 March 2020, pp. 36-40
-
- Article
- Export citation
-
Introduction:
Obsessive-compulsive disorder (OCD) is a highly disabling condition, with frequent early onset. Adult/adolescent OCD has been extensively investigated, but little is known about prevalence and clinical characterization of geriatric patients with OCD (G-OCD = 65 years). The present study aimed to assess prevalence of G-OCD and associated socio-demographic and clinical correlates in a large international sample.
Methods:Data from 416 outpatients, participating in the ICOCS network, were assessed and categorized into 2 groups, age < vs = 65 years, and then divided on the basis of the median age of the sample (age < vs = 42 years). Socio-demographic and clinical variables were compared between groups (Pearson Chi-squared and t tests).
Results:G-OCD compared with younger patients represented a significant minority of the sample (6% vs 94%, P < .001), showing a significantly later age at onset (29.4 ± 15.1 vs 18.7 ± 9.2 years, P < .001), a more frequent adult onset (75% vs 41.1%, P < .001) and a less frequent use of cognitive-behavioural therapy (CBT) (20.8% vs 41.8%, P < .05). Female gender was more represented in G-OCD patients, though not at a statistically significant level (75% vs 56.4%, P = .07). When the whole sample was divided on the basis of the median age, previous results were confirmed for older patients, including a significantly higher presence of women (52.1% vs 63.1%, P < .05).
Conclusions:G-OCD compared with younger patients represented a small minority of the sample and showed later age at onset, more frequent adult onset and lower CBT use. Age at onset may influence course and overall management of OCD, with additional investigation needed.
The effect of high maternal linoleic acid on endocannabinoid signalling in rodent hearts
- Simone L. Sleep, Nirajan Shrestha, James S. M. Cuffe, Olivia J. Holland, John P. Headrick, Andrew J. McAinch, Deanne H. Hryciw
-
- Journal:
- Journal of Developmental Origins of Health and Disease / Volume 11 / Issue 6 / December 2020
- Published online by Cambridge University Press:
- 09 December 2019, pp. 617-622
-
- Article
- Export citation
-
The endocannabinoid system (ECS), modulated by metabolites of linoleic acid (LA), is important in regulating cardiovascular function. In pregnancy, LA is vital for foetal development. We investigated the effects of elevated LA in H9c2 cardiomyoblasts in vitro and of a high linoleic acid (HLA, 6.21%) or low linoleic acid (LLA, 1.44%) diet during pregnancy in maternal and offspring hearts. H9c2 cell viability was reduced following LA exposure at concentrations between 300 and 1000 µM. HLA diet decreased cannabinoid receptor type 2 (CB2) mRNA expression in foetal hearts from both sexes. However, HLA diet increased CB2 expression in maternal hearts. The mRNA expression of fatty acid amide hydrolase (FAAH) in foetal hearts was higher in females than in males irrespective of diet and N-acyl phosphatidylethanolamine-specific phospholipase D (NAPE-PLD) mRNA expression showed an interaction between diet and sex. Data indicate that a high LA diet alters cell viability and CB2 expression, potentially influencing cardiac function during pregnancy and development of the offspring’s heart.
Automated Measurement of Maize Stalk Diameter and Plant Spacing
- J. S. Schepers, K. H. Holland, D. D. Francis
-
- Journal:
- Advances in Animal Biosciences / Volume 8 / Issue 2 / July 2017
- Published online by Cambridge University Press:
- 01 June 2017, pp. 220-223
- Print publication:
- July 2017
-
- Article
- Export citation
-
Crop phenotype is usually expressed in terms of characteristics like plant height, leaf architecture and leaf area index (LAI). In the case of maize, stalk diameter is seldom quantified because its measurement does not readily lend itself to automation. Justification for automating the measurement of stalk diameter and plant spacing is based on the finding that stalk diameter was able to account for about 65% of the variability in maize yield per plant in three irrigated field studies. A high-speed reflectance sensor and simulation apparatus was developed to explore the potential for automating maize stalk diameter assessment. The prototyped system accurately measured both stalk diameter and plant spacing in the laboratory at simulated velocities up to 12 km/h.
A Cognitive Aid for Anesthetic and Operating Room Management during a Hospital Power Failure
- Grete H. Porteous, Carli D. Hoaglan, Erica L. Holland, Martha A. Carlstead, Ryan P. Beecher, Bethany L. Tatachar, Chris J. Johnson
-
- Journal:
- Prehospital and Disaster Medicine / Volume 32 / Issue S1 / April 2017
- Published online by Cambridge University Press:
- 20 April 2017, p. S66
- Print publication:
- April 2017
-
- Article
-
- You have access Access
- Export citation
Large bilateral adrenal haemorrhages in a newborn with unrepaired cyanotic CHD
- Lerraughn M. Morgan, Erle H. Austin III, Brian J. Holland
-
- Journal:
- Cardiology in the Young / Volume 26 / Issue 5 / June 2016
- Published online by Cambridge University Press:
- 08 April 2016, pp. 1005-1007
-
- Article
- Export citation
-
Management of newborns with cyanotic CHD and bilateral adrenal haemorrhages has not previously been described in the literature. These abnormalities present unique challenges due to the potential for haemodynamic instability, need for open heart surgery and associated systemic anticoagulation in the newborn period, and the risk of catastrophic bleeding.
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
WCA Recommendations for the Long-Term Treatment of Obsessive-Compulsive Disorder in Adults
- John H. Greist, Borwin Bandelow, Eric Hollander, Donatella Marazziti, Stuart A. Montgomery, David J. Nutt, Ahmed Okasha, Richard P. Swinson, Joseph Zohar
-
- Journal:
- CNS Spectrums / Volume 8 / Issue S1 / August 2003
- Published online by Cambridge University Press:
- 07 November 2014, pp. 7-16
-
- Article
- Export citation
-
What are the latest psychotherapeutic and pharmacotherapeutic treatment recommendations for obsessive-compulsive disorder (OCD)? OCD is a relatively common disorder with a lifetime prevalence of ~2% in the general population. It often has an early onset, usually in childhood or adolescence, and frequently becomes chronic and disabling if left untreated. High associated healthcare utilization and costs, and reduced productivity resulting in loss of earning, pose a huge economic burden to OCD patients and their families, employers, and society. OCD is characterized by the presence of obsessions and compulsions that are time-consuming, cause marked distress, or significantly interfere with a person's functioning. Most patients with OCD experience symptoms throughout their lives and benefit from long-term treatment. Both psychotherapy and pharmacotherapy are recommended, either alone or in combination, for the treatment of OCD. Cognitive-behavioral therapy is the psychotherapy of choice. Pharmacologic treatment options include the tricyclic antidepressant clomipramine and the selective serotonin reuptake inhibitors (SSRIs) citalopram, fluoxetine, fluvoxamine, paroxetine, and sertraline. These have all shown benefit in acute treatment trials; clomipramine, fluvoxamine, fluoxetine, and sertraline have also demonstrated benefit in long-term treatment trials (at least 24 weeks), and clomipramine, sertraline, and fluvoxamine have United States Food and Drug Administration approvals for use in children and adolescents. Available treatment guidelines recommend first-line use of an SSR1 (ie, fluoxetine, fluvoxamine, paroxetine, sertraline, or citalopram) in preference to clomipramine, due to the latter's less favorable adverse-event profile. Further, pharmacotherapy for a minimum of 1–2 years is recommended before very gradual withdrawal may be considered.
Psychosocial Function and Economic Costs of Obsessive-Compulsive Disorder
- Eric Hollander, Dan J. Stein, Jee H. Kwon, Clayton Rowland, Cheryl M. Wong, James Broatch, Carol Himelein
-
- Journal:
- CNS Spectrums / Volume 2 / Issue 10 / December 1997
- Published online by Cambridge University Press:
- 07 November 2014, pp. 16-25
-
- Article
- Export citation
-
The study presented was conducted to analyze the effects of obsessive-compulsive symptoms on patients' quality of life and the costs incurred by patients and society for the treatment of obsessive-compulsive disorder (OCD). To accomplish this, a detailed 410-item questionnaire of psychosocial function and economic cost was sent to every fourth member of the Obsessive Compulsive Foundation. Of the 2,670 members who received the survey, 701 (26.9%) returned it.
Outcome measures included symptomatology, course of illness, impact of illness on psychosocial and other functioning, effects of diagnosis and treatment, and economic consequences. The demographics of this group were similar to those in smaller treatment-seeking clinical samples, but not necessarily to OCD sufferers within the US population as a whole. More than half of the patients reported moderate to severe interference in family relationships, socializing, and ability to study or work, secondary to OCD symptoms. A 10.2-year gap was observed between the onset of symptoms and the first attempt to seek professional help, and a 17.2-year gap was observed between the onset of symptoms and receipt of effective treatment. Specific treatments, such as serotonin reuptake inhibitors and behavior therapy showed greater symptom improvement, and significantly reduced the total annual fees incurred by OCD patients when compared with nonspecific treatments.
Our study results indicate that OCD has a profound effect on psychosocial functioning and quality of life. Large direct costs for OCD, and even larger indirect costs due to lost wages and underemployment were found. Greater awareness of OCD among practitioners may result in earlier diagnosis and more appropriate and cost-effective treatments.
WCA Recommendations for the Long-Term Treatment of Generalized Anxiety Disorder
- Christer Allgulander, Borwin Bandelow, Eric Hollander, Stuart A. Montgomery, David J. Nutt, Ahmed Okasha, Mark H. Pollack, Dan J. Stein, Richard P. Swinson
-
- Journal:
- CNS Spectrums / Volume 8 / Issue S1 / August 2003
- Published online by Cambridge University Press:
- 07 November 2014, pp. 53-61
-
- Article
- Export citation
-
What are the current recommendations for the long-term treatment of generalized anxiety disorder (GAD)? GAD is a common disorder with a lifetime prevalence of 4% to 7% in the general population. GAD is characterized by excessive, uncontrollable worry or anxiety about a number of events or activities that the individual experiences on more days than not over a 6-month period. Onset of GAD symptoms usually occurs during an individual's early twenties; however, high rates of GAD have also been seen in children and adolescents. The clinical course of GAD is often chronic, with 40% of patients reporting illness lasting >5 years. GAD is associated with pronounced functional impairment, resulting in decreased vocational function and reduced quality of life. Patients with GAD tend to be high users of outpatient medical care, which contributes significantly to healtcare costs. Currently, benzodiazepines and buspirone are prescribed frequently to treat GAD. Although both show efficacy in acute treatment trials, few long-term studies have been perform Benzodiazepines are not recommended for long-term treatment of GAD, due to associated development of tolerance, psychomotor impairment, cognitive and memory changes, physical dependence, and a withdrawal reaction on discontinuation. The antidepressant venlafaxine extended-release (XR) has received approval for the treatment of GAD in the United States and many other countries. Venlafaxine XR has demonstrated efficacy over placebo in two randomized treatment trials of 6 months' duration as well as in other acute trials. Paroxetine is the first of the selective serotonin reuptake inhibitors (SSRIs) to receive US approval for the treatment of GAD. Paroxetine demonstrated superiority to placebo in short-term trials, and investigations into the use of other SSRIs are ongoing. This suggests that other SSRIs, and serotonin and noradrenaline reuptake inhibitors, are likely to be effective in the treatment of GAD. Of the psychological therapies, cognitive-behavioral therapy (CBT) shows the greatest benefit in treating GAD patients. Treatment gains after a 12-week course of CBT may be maintained for up to 1 year. Currently, no guidelines exist for the long-term treatment of GAD.
WCA Recommendations for the Long-Term Treatment of Social Phobia
- Michael Van Ameringen, Christer Allgulander, Borwin Bandelow, John H. Greist, Eric Hollander, Stuart A. Montgomery, David J. Nutt, Ahmed Okasha, Mark H. Pollack, Dan J. Stein, Richard P. Swinson
-
- Journal:
- CNS Spectrums / Volume 8 / Issue S1 / August 2003
- Published online by Cambridge University Press:
- 07 November 2014, pp. 40-52
-
- Article
- Export citation
-
What is the best approach for treating patients with social phobia (social anxiety disorder) over the long term? Social phobia is the most common anxiety disorder, with reported prevalence rates of up to 18.7%. Social phobia is characterized by a marked and persistent fear of being observed or evaluated by others in social performance or interaction situations and is associated with physical, cognitive, and behavioral (ie, avoidance) symptoms. The onset of social phobia typically occurs in childhood or adolescence and the clinical course, if left untreated, is usually chronic, unremitting, and associated with significant functional impairment. Social phobia exhibits a high degree of comorbidity with other psychiatric disorders, including mood disorders, anxiety disorders, and substance abuse/dependence. Few people with social phobia seek professional help despite the existence of beneficial treatment approaches. The efficacy, tolerability, and safety of the selective serotonin reuptake inhibitors (SSRIs), evidenced in randomized clinical trials, support these agents as first-line treatment. The benzodiazepine clonazepam and certain monoamine oxidase inhibitors (representing both reversible and nonreversible inhibitors) may also be of benefit. Treatment of social phobia may need to be continued for several months to consolidate response and achieve full remission. The SSRIs have shown benefit in longterm treatment trials, while long-term treatment data from clinical studies of clonazepam are limited but support the drug's efficacy. There is also evidence for the effectiveness of exposure-based strategies of cognitive-behavioral therapy, and controlled studies suggest that the effects of treatment are generally maintained at long-term follow-up. In light of the chronicity and disability associated with social phobia, as well as the high relapse rate after short-term therapy, it is recommended that effective treatment be continued for at least 12 months.
Psychosocial Function and Economic Costs of Obsessive-Compulsive Disorder
- Eric Hollander, Dan J. Stein, Jee H. Kwon, Clayton Rowland, Cheryl M. Wong, James Broatch, Carol Himelein
-
- Journal:
- CNS Spectrums / Volume 3 / Issue S1 / May 1998
- Published online by Cambridge University Press:
- 07 November 2014, pp. 48-58
-
- Article
- Export citation
-
The study presented was conducted to analyze the effects of obsessive-compulsive symptoms on patients' quality of life and the costs incurred by patients and society for the treatment of obsessive-compulsive disorder (OCD). To accomplish this, a detailed 410-item questionnaire of psychosocial function and economic cost was sent to every fourth member of the Obsessive Compulsive Foundation. Of the 2,670 members who received the survey, 701 (26.9%) returned it.
Outcome measures included symptomatology, course of illness, impact of illness on psychosocial and other functioning, effects of diagnosis and treatment, and economic consequences. The demographics of this group were similar to those in smaller treatment-seeking clinical samples, but not necessarily to OCD sufferers within the US population as a whole. More than half of the patients reported moderate to severe interference in family relationships, socializing, and ability to study or work, secondary to OCD symptoms. A 10.2-year gap was observed between the onset of symptoms and the first attempt to seek professional help, and a 17.2-year gap was observed between the onset of symptoms and receipt of effective treatment. Specific treatments, such as serotonin reuptake inhibitors and behavior therapy, showed greater symptom improvement, and significantly reduced the total annual fees incurred by OCD patients when compared with nonspecific treatments.
Our study results indicate that OCD has a profound effect on psychosocial functioning and quality of life. Large direct costs for OCD and even larger indirect costs due to lost wages and underemployment were found. Greater awareness of OCD among practitioners may result in earlier diagnosis and more appropriate and cost-effective treatments.
WCA Recommendations for the Long-Term Treatment of Posttraumatic Stress Disorder
- Dan J. Stein, Borwin Bandelow, Eric Hollander, David J. Nutt, Ahmed Okasha, Mark H. Pollack, Richard P. Swinson, Joseph Zohar
-
- Journal:
- CNS Spectrums / Volume 8 / Issue S1 / August 2003
- Published online by Cambridge University Press:
- 07 November 2014, pp. 31-39
-
- Article
- Export citation
-
Posttraumatic stress disorder (PTSD) is a common and disabling condition. In addition to combat-related PTSD, the disorder occurs in civilians exposed to severe traumatic events, with the community prevalence rate for the combined populations reaching as high as 12%. If left untreated, PTSD may continue for years after the stressor event, resulting in severe functional and emotional impairment and a dramatic reduction in quality of life, with negative economic consequences for both the sufferer and society as a whole. Although PTSD is often overlooked, diagnosis is relatively straight-forward once a triggering stressor event and the triad of persistent symptoms—reexperiencing the traumatic event, avoiding stimuli associated with the trauma, and hyperarousal—have been identified. However, comorbid conditions of anxiety and depression frequently hamper accurate diagnosis. Treatment for PTSD includes psychotherapy and pharmacotherapy. The latter includes selective serotonin reuptake inhibitors (SSRIs), tricyclic antidepressants, and monoamine oxidase inhibitors. Only SSRls have been proven effective and safe in long-term randomized controlled trials. Current guidelines from the Expert Consensus Panel for PTSD recommend treatment of chronic PTSD for a minimum of 12–24 months.
WCA Recommendations for the Long-Term Treatment of Panic Disorder
- Mark H. Pollack, Christer Allgulander, Borwin Bandelow, Giovanni B. Cassano, John H. Greist, Eric Hollander, David J. Nutt, Ahmed Okasha, Richard P. Swinson
-
- Journal:
- CNS Spectrums / Volume 8 / Issue S1 / August 2003
- Published online by Cambridge University Press:
- 07 November 2014, pp. 17-30
-
- Article
- Export citation
-
What are the symptoms of panic disorder and how is the disorder most effectively treated? One of the most commonly encountered anxiety disorders in the primary care setting, panic disorder is a chronic and debilitating illness. The core symptoms are recurrent panic attacks coupled with anticipatory anxiety and phobic avoidance, which together impair the patient's professional, social, and familial functioning. Patients with panic disorder have medically unexplained symptoms that lead to overutilization of healthcare services. Panic disorder is often comorbid with agoraphobia and major depression, and patients may be at increased risk of cardiovascular disease and, possibly, suicide. Research into the optimal treatment of this disorder has been undertaken in the past 2 decades, and numerous randomized, controlled trials have been published. Selective serotonin reuptake inhibitors have emerged as the most favorable treatment, as they have a beneficial side-effect profile, are relatively safe (even if taken in overdose), and do not produce physical dependency. High-potency benzodiazepines, reversible monoamine oxidase inhibitors, and tricyclic antidepressants, have also shown antipardc efficacy. In addition, cognitive-behavioral therapy has demonstrated efficacy in the acute and long-term treatment of panic disorder. A n integrated treatment approach that combines pharmacotherapy with cognitive-behavioral therapy may provide the best treatment. Long-term efficacy and ease of use are important considerations in treatment selection, as maintenance treatment is recommended for at least 12–24 months, and in some cases, indefinitely.
Contributors
-
- By Michael H. Allen, Leora Amira, Victoria Arango, David W. Ayer, Helene Bach, Christopher R. Bailey, Ross J. Baldessarini, Kelsey Ball, Alan L. Berman, Marian E. Betz, Emily A. Biggs, R. Warwick Blood, Kathleen T. Brady, David A. Brent, Jeffrey A. Bridge, Gregory K. Brown, Anat Brunstein Klomek, A. Jacqueline Buchanan, Michelle J. Chandley, Tim Coffey, Jessica Coker, Yeates Conwell, Scott J. Crow, Collin L. Davidson, Yogesh Dwivedi, Stacey Espaillat, Jan Fawcett, Steven J. Garlow, Robert D. Gibbons, Catherine R. Glenn, Deborah Goebert, Erica Goldstein, Tina R. Goldstein, Madelyn S. Gould, Kelly L. Green, Alison M. Greene, Philip D. Harvey, Robert M. A. Hirschfeld, Donna Holland Barnes, Andres M. Kanner, Gary J. Kennedy, Stephen H. Koslow, Benoit Labonté, Alison M. Lake, William B. Lawson, Steve Leifman, Adam Lesser, Timothy W. Lineberry, Amanda L. McMillan, Herbert Y. Meltzer, Michael Craig Miller, Michael J. Miller, James A. Naifeh, Katharine J. Nelson, Charles B. Nemeroff, Alexander Neumeister, Matthew K. Nock, Jennifer H. Olson-Madden, Gregory A. Ordway, Michael W. Otto, Ghanshyam N. Pandey, Giampaolo Perna, Jane Pirkis, Kelly Posner, Anne Rohs, Pedro Ruiz, Molly Ryan, Alan F. Schatzberg, S. Charles Schulz, M. Katherine Shear, Morton M. Silverman, April R. Smith, Marcus Sokolowski, Barbara Stanley, Zachary N. Stowe, Sarah A. Struthers, Leonardo Tondo, Gustavo Turecki, Robert J. Ursano, Kimberly Van Orden, Anne C. Ward, Danuta Wasserman, Jerzy Wasserman, Melinda K. Westlund, Tracy K. Witte, Kseniya Yershova, Alexandra Zagoloff, Sidney Zisook
- Edited by Stephen H. Koslow, University of Miami, Pedro Ruiz, University of Miami, Charles B. Nemeroff, University of Miami
-
- Book:
- A Concise Guide to Understanding Suicide
- Published online:
- 05 October 2014
- Print publication:
- 18 September 2014, pp vii-x
-
- Chapter
- Export citation